What’s New in Pediatric Dermatology?
Yvonne E. Chiu, MD, Professor of Dermatology and Pediatrics, Vice Chair and Medical Director, Pediatric Dermatology, Medical College of Wisconsin
December 2022
Dr. Chiu presented several cases to display what’s new in pediatric dermatology. Because many patients have limited access to pediatric dermatology care, her goal is to help other dermatologists become more comfortable caring for children.
The first case was a four-month-old infant with a hemangioma on the breast. Dr. Chiu asked the audience if they would recommend propranolol or timolol. The use of propranolol to treat infantile hemangiomas was first reported in 2008. In 2013, Dr. Chiu and a multi-disciplinary group convened to develop consensus recommendations on propranolol. Since then, studies showed that propranolol was safer and easier to use than originally thought with rare serious adverse events. Other studies showed that timolol may also not be as safe. Dr. Chiu recommended that general dermatologists become more comfortable using propranolol for low-risk infants and referring high-risk infants to pediatric dermatologists.
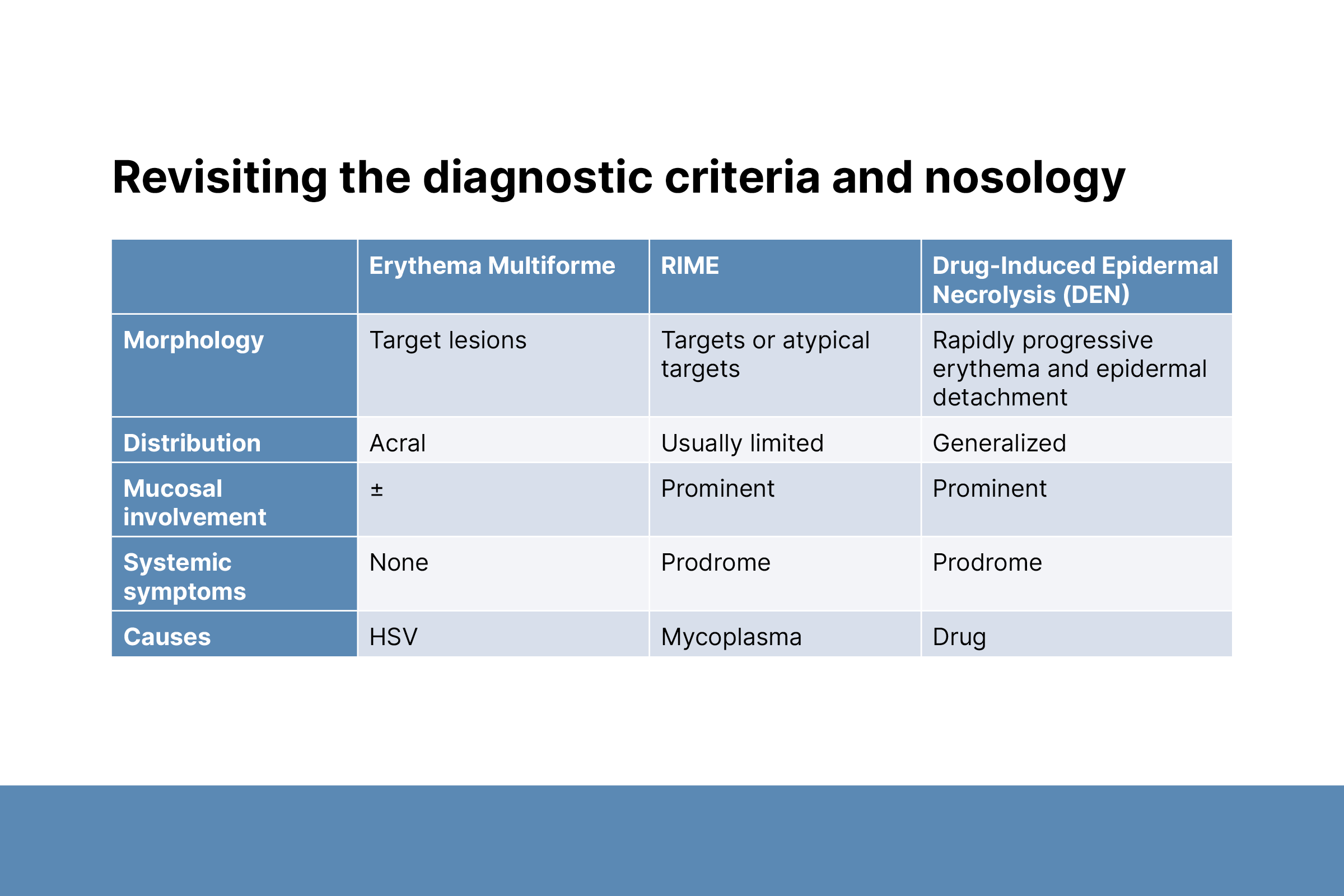
The second case was an eight-year-old boy with oral ulcers, lip erosions, fevers, myalgia, cough, conjunctival erythema, and very few skin findings, including small erosions on the finger and arm. The diagnosis was reactive infectious mucocutaneous eruption. This newly recognized disease has similar clinical manifestations to Stevens-Johnson syndrome but has a much better prognosis.
The third case was a three-year-old girl who had had a red rash for a year and tiny red macules on her thigh, shoulder, chest, and hands. Genetic analysis determined that she had heterozygous mutations in RASA1 and EPHB4. The diagnosis was a capillary malformation-arteriovenous malformation CM-AVM syndrome, which was first described in 2003. Dr. Chiu’s final takeaway message was to beware of the small brown capillary malformations of CM-AVM syndrome. These patients can have visceral AVMs and early diagnosis and treatment is important.